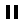Anterior Hip Replacement
Anterior Hip Replacement
Total Hip Replacement
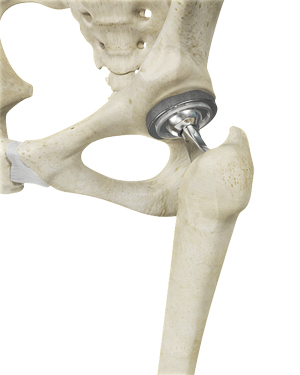
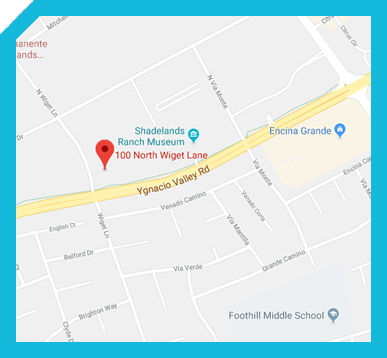
Total hip replacement is a surgical procedure in which the damaged cartilage and bone is removed from the hip joint and replaced with artificial components. The hip joint is one of the body's largest weight-bearing joints, located between the thigh bone (femur) and the pelvis (acetabulum). It is a ball and socket joint in which the head of the femur is the ball and the pelvic acetabulum forms the socket. The joint surface is covered by a smooth articular cartilage which acts as a cushion and enables smooth movements of the joint.
Several diseases and conditions can cause damage to the articular cartilage. Total hip replacement surgery is an option to relieve severe arthritis pain that limits your daily activities.
Disease Overview
Arthritis is inflammation of the joints resulting in pain, swelling, stiffness and limited movement. Hip arthritis is a common cause of chronic hip pain and disability. The three most common types of arthritis that affect the hip are:
- Osteoarthritis: It is characterized by progressive wearing away of the cartilage of the joint. As the protective cartilage wears down, the bone ends rub against each other and cause pain in the hip. Rheumatoid arthritis: This is an autoimmune disease in which the tissue lining the joint (synovium) becomes inflamed, resulting in the production of excessive joint fluid (synovial fluid). This leads to loss of cartilage causing pain and stiffness.
- Traumatic arthritis: This is a type of arthritis resulting from a hip injury or fracture. Such injuries can damage the cartilage and cause hip pain and stiffness over a period.
Symptoms
The most common symptom of hip arthritis is joint pain and stiffness resulting in limited range of motion. Vigorous activity can increase the pain and stiffness which may cause limping while walking.
Diagnosis
Diagnosis is made by evaluating medical history, physical examination and X-rays.
Surgical Procedure
Surgery may be recommended, if conservative treatment options such as anti-inflammatory medications and physical therapy do not relieve the symptoms.
The surgery is performed under general anesthesia. During the procedure, a surgical cut is made over the hip to expose the hip joint and the femur is dislocated from the acetabulum. The surface of the socket is cleaned and the damaged or arthritic bone is removed using a reamer. The acetabular component is inserted into the socket using screws or occasionally bone cement. A liner made of plastic, ceramic or metal is placed inside the acetabular component. The femur or thigh bone is then prepared by removing the arthritic bone using special instruments, to exactly fit the new metal femoral component. The femoral component is then inserted to the femur either by a press fit or using bone cement. Then the femoral head component made of metal or ceramic is placed on the femoral stem. All the new parts are secured in place using special cement. The muscles and tendons around the new joint are repaired and the incision is closed.
Post-operative care
After undergoing total hip replacement, you must take special care to prevent the new joint from dislocating and to ensure proper healing. Some of the common precautions to be taken include:
- Avoid combined movement of bending your hip and turning your foot inwards
- Keep a pillow between your legs while sleeping for 6 weeks
- Never cross your legs and bend your hips past a right angle (90)
- Avoid sitting on low chairs
- Avoid bending down to pick up things, instead a grabber can be used to do so
- Use an elevated toilet seat
Risks
As with any major surgical procedure, there are certain potential risks and complications involved with total hip replacement surgery. The possible complications after total hip replacement include:
- Infection
- Dislocation
- Fracture of the femur or pelvis
- Injury to nerves or blood vessels
- Formation of blood clots in the leg veins
- Leg length inequality
- Hip prosthesis may wear out
- Failure to relieve pain
- Scar formation
- Pressure sores
Total hip replacement is one of the most successful orthopaedic procedures performed for patients with hip arthritis. This procedure can relieve pain, restore function, improve your movements at work and play, and provide you with a better quality of life.
MAKOPlasty Total Hip Replacement
Degenerative joint disease (DJD), a common cause of hip pain, is a chronic condition hampering the quality of life of affected individuals. There are different types of DJD and the most common ones include osteoarthritis (OA), post-traumatic arthritis, rheumatoid arthritis (RA), avascular necrosis (AVN), and hip dysplasia.
MAKOplasty® Total Hip Replacement is a novel surgical alternative for patients with degenerative joint disease (DJD). In this procedure, a Robotic Arm Interactive Orthopedic System (RIO®) assists the surgeon in aligning and positioning implants more precisely.
MAKOplasty can be considered in patients with pain while bearing weight on the affected joint, pain or stiffness in the hip while walking or performing other activities, and also in patients not responding to a conservative line of management.
MAKOPlasty procedure

Accurate placement and alignment of the hip implant is crucial in hip replacement surgery. MAKOplasty® Total Hip Replacement utilizes a CT scan of the patient’s hip to generate a 3-D model of their pelvis and femur. These aid the surgeon in planning your surgery.
During surgery, the RIO® software provides dynamic information to enhance accuracy of the procedure. Such real-time information assists the surgeon in precise placement of the implant, which can be difficult to achieve with traditional surgical techniques.
- Precise placement of the hip implant using the surgeon-controlled robotic arm system with a decline in the possible risk of hip dislocation
- Uniformity in leg length, reducing the requirement of a shoe lift
- Increased longevity of the implant due to a reduction in abnormal rubbing between implant and bone
Robotic Arm Interactive Orthopedic System (RIO®)
RIO® Features:
- Accurately plan implant size, orientation and alignment utilizing CT-derived 3-D modelling
- Enabling the pre-resection capture of patient-specific kinematic tracking through full flexion and extension
- Real-time intra-operative adjustments for correct hip kinematics and soft-tissue balance
- Minimally invasive and bone sparing, with minimal tissue trauma for faster recovery
Direct Anterior Approach Total Hip Replacement
by Amir Jamali, MD
Last updated 4/29/2017Total Hip Replacement
Total hip arthroplasty is one of the most successful medical procedures ever invented. Approximately 300,000 such procedures are performed in the United States annually. This procedure can treat a wide variety of disorders that ultimately lead to severe arthritis of the hip. Arthritis is characterized by destruction of the articular cartilage and direct contact of the bony surfaces of the hip socket and femoral head. This can lead to pain, stiffness, inability to walk, difficulty sitting, and other disabilities. The main goal of total hip replacement is to relieve pain. However, many patients have the ability to walk farther after the procedure and often no longer require walking aids after the surgery.
The procedure is usually performed under a general or spinal anesthesia. The procedure can be performed with the patient either lying on their side or on their back. The hip can be approached from the front, the back, or the side. After the hip is exposed, the neck of the femur is cut at a specific angle and the femoral head is removed. This allows a good view into the hip socket. The arthritic hip socket often has lost its cartilage and has developed many bone spurs. A device known as a reamer is used to prepare the hip socket for a metal cup by machining it to a hemispherical shape and exposing a bleeding surface of bone to allow ingrowth of bone onto the hip socket component (acetabular component). Next, the component is impacted into place. Once the acetabular component has been applied, a second component or prosthesis is placed into the femoral shaft. The femoral component is usually composed of titanium or cobalt-chromium alloy. Depending on the specific design, it can be implanted with bone cement or with direct contact to the bone (press-fit).
TOTAL HIP REPLACEMENT (ANTERIOR APPROACH)
The following case is an illustration of the steps involved in a total hip replacement performed in a 29 year old female with severe avascular necrosis of the femoral head and secondary arthritis.
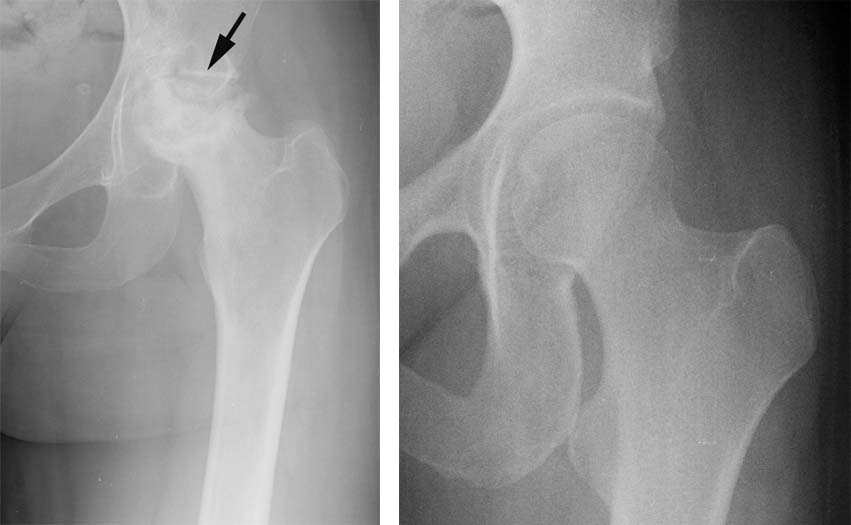
1.This patient's hip radiograph (left) demonstrates the advanced avascular necrosis of the femoral head. This is shown as flattening and fragmentation of the upper aspect of the femoral head. At the time of the radiograph, we also notice that she has developed flattening at the edge of the hip socket (arrow). A normal hip radiograph is shown immediately below the patient's hip radiograph.
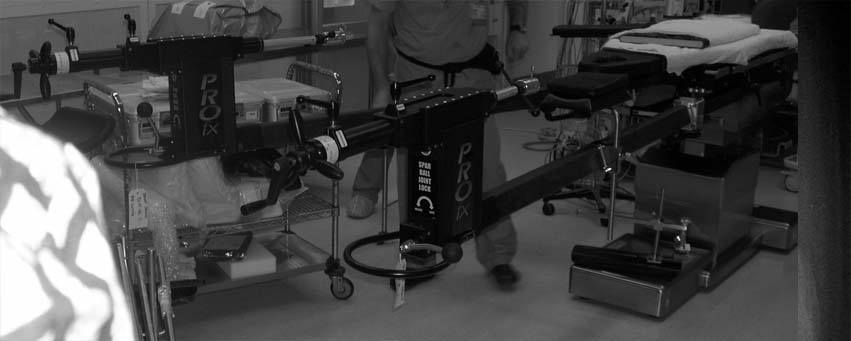
2.A special operating room table is used to position the leg in order to facilitate the surgical exposure. The table allows the leg to be bent toward the floor to allow direct access to the top of the femur (thighbone) through the incision in the front.
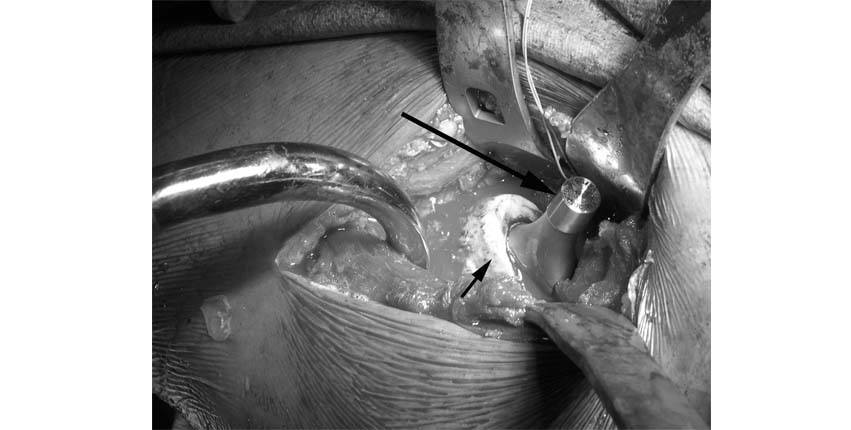
3.A specialized hook is attached to the table which helps to hold the femur up while a titanium stem is placed within the upper part of the femur. In this image the prosthesis or metal stem(long arrow) has been seated fully into the femur with the neck of the prosthesis coming out toward the camera(short arrow).

4.A ceramic femoral head component has been mounted onto the metal femoral component. The ceramic head component is spherical and measures 36mm in this case. The femoral head fits into a precisely matched ceramic insert which locks into the hip socket component (acetabular component). The combination of the femoral head and the insert makes up the "bearing surface" which in this case is ceramic on ceramic.
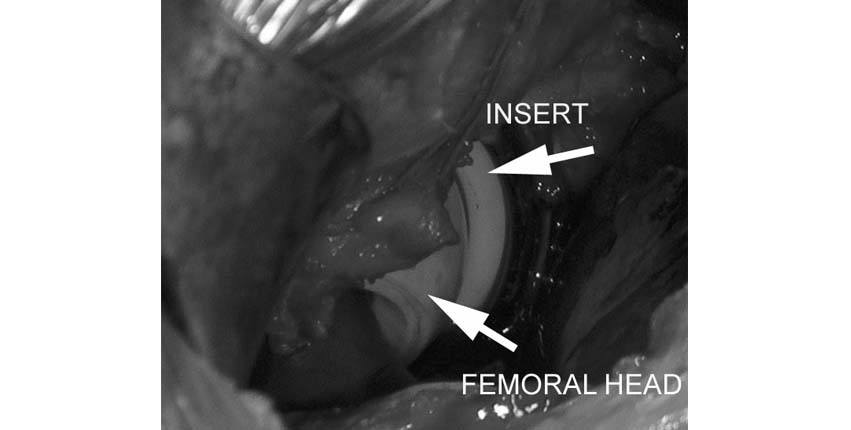
5.At this point the femoral head has been placed in the hip socket component. The hip is now "reduced" (put back in place). A final check of the position of the hip implants is performed. The leg is moved in extreme positions to be sure that the hip implants do not come apart due to dislocation. Potential reasons for the hip to dislocate would be abnormal contact between the implants, inaccurate positioning of the implants, or inadequate soft tissue (muscle) tension.
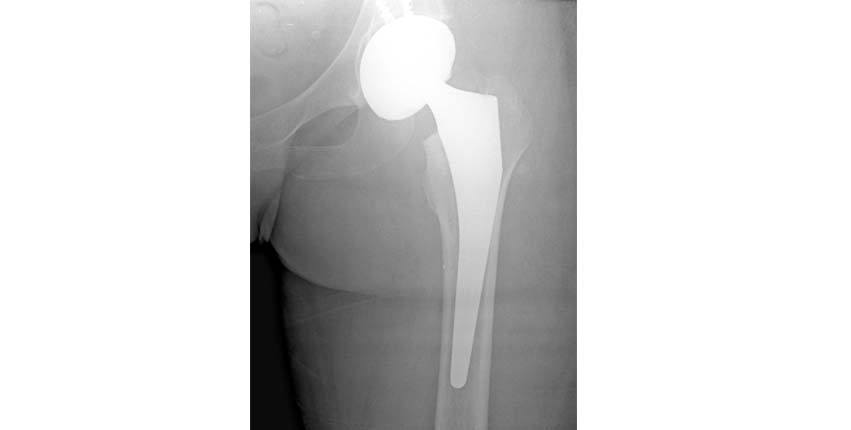
6.The final radiograph shows the implants to be in appropriate position.
FAQ Total Hip Replacement
What are current hip replacements made of?
Most contemporary metal hip replacements are made of titanium alloys or cobalt-chromium alloys. The best way to understand the implants used in current replacements is to divide them into two parts. First is the metallic components that are directly fixed to the bone. These can be either through the use of cement (mostly on the femur or thigh-bone) or through a cementless or ingrowth process where the bone actually grows onto the metal. The second part of the hip replacement is made of the parts that actually move relative to one another (the bearing). These can be made of either metal on polyethylene plastic (most common) or other bearings such as ceramic-on-ceramic or metal-on-metal.
How long will I be in the hospital?
In most cases, patients remain in the hospital at our facility for a minimum of 2 days and usually 3-4 days.
Would I go home or go to a nursing facility after the surgery?
This depends on how much help you have at home. The goal of physical therapy both in the hospital and at home is to get you to be independent. If this can not be acheived while you are in the hospital, a vigorous course of therapy in a skilled nursing facility is the best answer to continue to progress toward independence.
Can I put my full weight on the leg after a hip replacement?
In most cases of ingrowth prostheses, we restrict the amound of weightbearing on the leg for 4 to 6 weeks. This has been shown to lead to decreased risk of the stem collapsing into the femur
What does the term “bearing surface” mean?
Bearing surface refers to the surfaces that actually contact one another in a total hip replacement. The ideal bearing surface for a joint is cartilage. This is a result of its electrical properties, water content, and architecture. As a result, cartilage on cartilage has a lower friction than ice on ice. In total joint replacement, the goal is to achieve a low friction joint with production of as little debris as possible and provides long-term durability to last the patient’s lifetime. The various current options for bearing surfaces in joint replacement include metal-on-polyethylene, ceramic-on-ceramic, and metal-on-metal.
When do you use bone cement?
Bone cement has had a long history of use in total hip replacement. Over the past 15 years, its use has declined due to the risk associated with loosening of cemented joint replacements. In our efforts to improve on the results of the cemented joint replacements, a number of cementless implants have been developed. Cementless implants depend on the ingrowth or ongrowth of bone onto their surface. The various surfaces can be made of a roughened surface, a surface with small beads, or a fibrous metal mesh. The cementless implants on the socket side have performed exceedingly well. A number of earlier cementless implants on the femoral side did not perform as well as cemented femoral components. However, we have learned important lessons about factors that are associated with success in cementless femoral components. Currently, a number of published reports have shown that some cementless femoral and acetabular designs have a 98 to 100% success rate at 10 years. These are equal or better to many cemented designs at the same time intervals. We currently use predominantly cementless designs unless we are concerned about the fixation of such implants. In such cases, cemented implants offer immediate fixation to bone and permit immediate weightbearing for the patient.
Do hips wear out?
Total hip replacements can wear out. This has been associated with higher activity, with polyethylenes with poor mechanical properties, and with larger diameter femoral heads. Currently, with bearing surfaces such as highly cross-linked polyethylenes, metal-on-metal, and ceramic-on-ceramic, the rates of wear in hip replacements may finally be controlled.
Can I jog after my hip replacement?
No published study has documented the clinical outcome of hip replacements in patients who are runners. However, the association of higher failure rates with younger, more active patients suggest that such activities may lead to an earlier need for revision surgery.
Do I have to follow any other precautions after my surgery?
Depending on the approach, there will be certain precautions/positions to avoid after hip replacement. For most posterior approaches, the patient is asked to avoid bending their hip greater than 90 degrees, to avoid turning their knee in (internal rotation) during activities like picking up an object from the floor, and to avoid deep, cushioned couches. Anterior or lateral hip approaches often require anterior hip precautions (no turning out of the foot while standing or lying flat).
Will my leg lengths be equal after the surgery?
Your surgeon will make efforts to achieve equal leg lengths after the surgery. The most important factor in success after total hip replacement is the achievement of a stable hip (a hip that does not dislocate). The stability of the hip depends on the positioning of the implants, the tightness of the soft-tissues, and the bony anatomy. In some cases, the leg needs to lengthened slightly in order to achieve adequate soft-tissue tension.
What would happen if my hip dislocates?
A dislocated hip can occur during activities in which the precautions are not followed or as a result of soft-tissue laxity or impingement. Impingement is a situation where the component or bony structures contact each other in such a way that they push the hip out of socket.
What is the "anterior approach total hip replacement"?
The anterior approach for total hip replacement is a surgical approach to the hip that has been used for over 30 years for total hip replacement in Europe and more recently in the United States. The major advantage of the surgery is that it provides a truly "minimally invasive" way to perform the hip replacement. The muscular interval between the tensor fasciae latae muscle and the sartorius muscle is used. No muscle is cut with the operation, providing a very stable hip with minimal damage to the soft-tissues of the hip. There are no bending or positional precautions after the surgery. We use a special table called a "fracture table" to perform the operation. It allows us to position the leg during the operation and helps to expose both the socket and the femur.
What if I have a car accident with a hip replacement? Can the bone break around the replacement?
Yes, trauma of any kind after a hip replacement can lead to very severe fractures which are even harder to treat that a fracture without a hip replacement. The treatment of these injuries often requires either the use of plates and rods or the revision of the hip replacement entirely with placement of a new, long femoral component to span the fracture.
What is resurfacing total hip replacement?
Resurfacing total hip replacement is a type of hip replacement that places the femoral component on the neck of the femur rather than passing a stem down the shaft. The cup component in the hip socket is usually a one piece all metal component.
Do you have any cartilage replacement procedures for the hip?
At this point the experience with the treatment of cartilage defects in the hip is limited to a few scattered reports. These include the use of microfracture, mosaicplasty, and osteochondral allografting. The challenge in the hip is the difficulty in accessing the joint, the specific geometry of the ball and socket, and the limited blood supply of the head of the femur.
Please download our Direct Anterior Approach Total Hip Replacement Brochure for further information.
- Barton C, Kim PR. Complications of the direct anterior approach for total hip arthroplasty. Orthop Clin North Am. Jul 2009;40(3):371-375.
- Bender B, Nogler M, Hozack WJ. Direct anterior approach for total hip arthroplasty. Orthop Clin North Am. Jul 2009;40(3):321-328.
- Bhandari M, Matta JM, Dodgin D, et al. Outcomes following the single-incision anterior approach to total hip arthroplasty: a multicenter observational study. Orthop Clin North Am. Jul 2009;40(3):329-342.
- Nakata K, Nishikawa M, Yamamoto K, Hirota S, Yoshikawa H. A clinical comparative study of the direct anterior with mini-posterior approach: two consecutive series. J Arthroplasty. Aug 2009;24(5):698-704.
- Rachbauer F, Kain MS, Leunig M. The history of the anterior approach to the hip. Orthop Clin North Am. Jul 2009;40(3):311-320.
- Restrepo C, Parvizi J, Pour AE, Hozack WJ. Prospective randomized study of two surgical approaches for total hip arthroplasty. J Arthroplasty. Aug 2010;25(5):671-679 e671.
- 7Auffarth A, Resch H, Lederer S, et al. Does the choice of approach for hip hemiarthroplasty in geriatric patients significantly influence early postoperative outcomes? A randomized-controlled trial comparing the modified Smith-Petersen and Hardinge approaches. J Trauma. May 2011;70(5):1257-1262.
- Baba T, Shitoto K, Kaneko K. Bipolar hemiarthroplasty for femoral neck fracture using the direct anterior approach. World J Orthop. Apr 18 2013;4(2):85-89.
- Barrett WP, Turner SE, Leopold JP. Prospective randomized study of direct anterior vs postero-lateral approach for total hip arthroplasty. J Arthroplasty. Oct 2013;28(9):1634-1638.
- Martin CT, Pugely AJ, Gao Y, Clark CR. A comparison of hospital length of stay and short-term morbidity between the anterior and the posterior approaches to total hip arthroplasty. J Arthroplasty. May 2013;28(5):849-854.
- Poehling-Monaghan KL, Kamath AF, Taunton MJ, Pagnano MW. Direct Anterior versus Miniposterior THA With the Same Advanced Perioperative Protocols: Surprising Early Clinical Results. Clin Orthop Relat Res. Aug 1 2014.
- Post ZD, Orozco F, Diaz-Ledezma C, Hozack WJ, Ong A. Direct Anterior Approach for Total Hip Arthroplasty: Indications, Technique, and Results. J Am Acad Orthop Surg. Sep 2014;22(9):595-603.
- Rathod PA, Orishimo KF, Kremenic IJ, Deshmukh AJ, Rodriguez JA. Similar improvement in gait parameters following direct anterior & posterior approach total hip arthroplasty. J Arthroplasty. Jun 2014;29(6):1261-1264.
- Taunton MJ, Mason JB, Odum SM, Springer BD. Direct anterior total hip arthroplasty yields more rapid voluntary cessation of all walking AIDS: a prospective, randomized clinical trial. J Arthroplasty. Sep 2014;29(9 Suppl):169-172.
- Unger AC, Dirksen B, Renken FG, Wilde E, Willkomm M, Schulz AP. Treatment of femoral neck fracture with a minimal invasive surgical approach for hemiarthroplasty - clinical and radiological results in 180 geriatric patients. Open Orthop J. 2014;8:225-231.
- Zawadsky MW, Paulus MC, Murray PJ, Johansen MA. Early outcome comparison between the direct anterior approach and the mini-incision posterior approach for primary total hip arthroplasty: 150 consecutive cases. J Arthroplasty. Jun 2014;29(6):1256-1260.