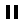Hip Resurfacing
Hip Resurfacing
Birmingham Hip Resurfacing
The Birmingham Hip Resurfacing (BHR) is a metal-on-metal prosthesis used in hip resurfacing procedure. Hip Resurfacing is a bone conserving procedure where the acetabulum (hip socket) is replaced and femoral head is resurfaced. Hip resurfacing is indicated in all the individuals with arthritis where conservative treatment was a failure. Advantage of hip resurfacing procedure is that the little bone is removed from femoral head and this spares the femoral canal.
The conventional method of total hip replacement offers poor long-term outcomes for young and active patients leading to the further complications such as revision surgery and associated problems.
In hip resurfacing, the articular surfaces of the femur and acetabulum are replaced. The procedure is bone conserving as most of the head of the femur is retained. Instead of removing the head completely as with a total hip replacement, it is shaped to accept a low-wear metal sphere. This sphere matches the patient's own anatomy that confers low risk of dislocation, a broad range of movement and excellent stability. A comprehensive range of sizes is offered to address the needs of almost all patients, and those with acetabular deficiencies.
The BHR offers a bone conserving, less invasive alternative to total hip replacement, with the potential for higher levels of patient activity. The BHR device is designed to suit cemented fixation or cement-less press-fit fixation. The resurfacing femoral head and acetabular cups are available in various sizes to suit everyone’s needs. The BHR system has allowed many young and active patients, athletes, and sports personalities with arthritic hip to perform their normal activities with no or minimal pain. It can be used in all individuals aged <60 years and in individuals aged>60 years with bone quality strong enough to support the implant.
(Total Hip Resurfacing, Surface Replacement Arthroplasty)
by Amir Jamali, MD
Last updated 4/29/2017Total hip resurfacing arthroplasty is a type of total hip replacement where the femoral component is placed upon the femoral neck. This is in contrast to standard hip replacements where the femoral neck is cut and a stem is placed into the proximal femur. The bearing surfaces (the pieces that contact one another) for current resurfacing total hip replacements are metal and are machined to very high tolerances to minimize the amount of debris in the joint. These so called “metal on metal” bearings are also used with some standard total hip replacements. Metal on metal bearings have been used in total hip replacement for greater than 30 years. Studies have shown that metal on metal bearings produce detectable amounts of ions in the liver, kidney, and urine. In spite of this, there have been no cases of cancer reported as a result of the metal on metal hip replacements up to now. Metal on metal bearings allow the surgeon to use larger diameter femoral and acetabular components which leads to a improved range of motion and potentially a lower dislocation rate. The additional benefit (and more important benefit) of resurfacing total hip replacement is the preservation of native bone in the femur. This would minimize the risk of debris traveling down the bone leading to bone digestion (osteolysis). Also, if a patient with a resurfacing total hip has a fracture of the neck of the femur, in many cases, the hip can be treated with conversion to a standard total hip replacement. However, this benefit does come at a cost.
Potential Complications
The major problems with resurfacing include the requirement of using a metal on metal bearing, the risk of loosening of the femoral component (in cases of large cysts or inadequate bone), and the technical difficulty of the surgery. The surgery is more challenging since the femoral neck remains intact and can obstruct the view of the hip socket (acetabulum). Not all patients are candidates for resurfacing total hip replacement. In particular, patients who have large cysts in the femoral head or hip socket, low bone density, those with a great degree of deformity, or extensive bone spurs around the hip socket would be best treated with a standard hip replacement. Other complications include infection, nerve injury, fracture of the femoral neck beneath the resurfacing implant, impingement or abnormal contact between the neck of the femur and the edge of the cup, loosening of the implants, and persistent pain.
CLINICAL CASE: RESURFACING TOTAL HIP REPLACEMENT
The following case is an illustration of the steps involved in a resurfacing total hip replacement performed in a 58 year old male with osteoarthritis of the right hip.
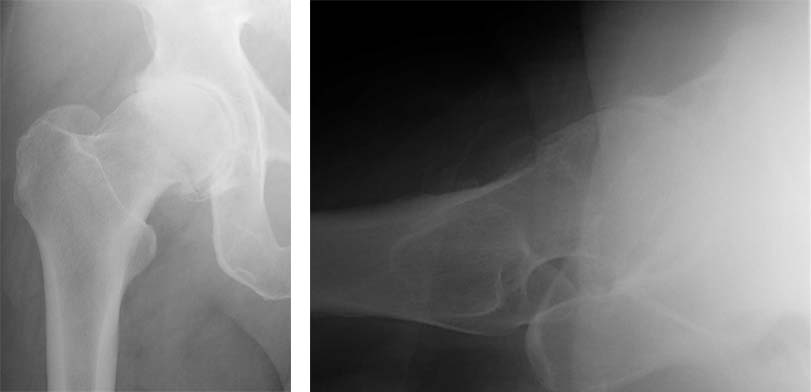
1.These radiographs show advances arthritis of the right hip. The architecture of the femoral head is consistent with femoroacetabular impingement as the underlying cause of the osteoarthritis. The patient elected to have right hip resurfacing total hip replacement.
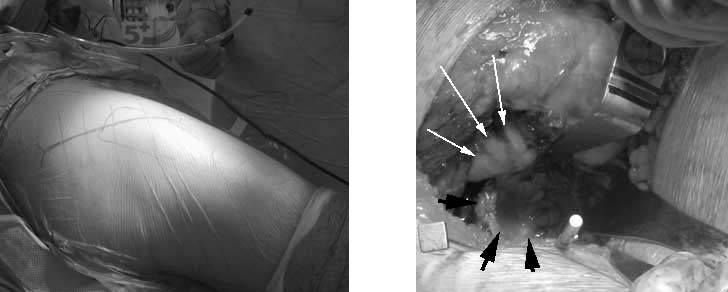
2.A posterior approach to the hip was selected. The patient is positioned with his left side down and is fixed to the table using supports. The hip is approached with release of the soft-tissues to allow the femoral head to be retracted forward, exposing the hip socket.ral neck, a cylindrical reamer is passed over the femoral head, removing bone at the periphery of the femoral head.

3.After the femoral head is exposed and a guidepin is passed down the shaft of the femoral neck, a cylindrical reamer is passed over the femoral head, removing bone at the periphery of the femoral head.

4.After removal of this device and placement of the cup the head is inspected to be sure that all peripheral bone has been removed. Next a special reamer device is passed over the head in order to shape it to match the inside of the femoral resurfacing implant.

5.Next, drill holes are made at the top of the head and on the edges to maximize cement fixation onto the femoral head and neck.
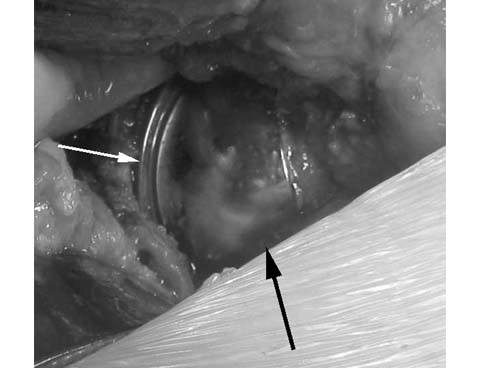
6.The femoral component is cemented into place. In the photograph, above the femoral (large black arrow) and acetabular components (small white arrow) are mated and the femoral head is placed within the socket. The range of motion is checked at this point in the surgery.

7.These final radiographs show the implants in the desired position and alignment.
FAQ Total Hip Resurfacing Arthroplasty
1. What is the difference between a standard hip replacement and a resurfacing total hip replacement?
Most contemporary metal hip replacements are made of titanium alloys or cobalt-chromium alloys. The best way to understand the implants used in current replacements is to divide them into two parts. First is the metallic components that are directly fixed to the bone. These can be either through the use of cement (mostly on the femur or thigh-bone) or through a cementless or ingrowth process where the bone actually grows onto the metal. The second part of the hip replacement is made of the parts that actually move relative to one another (the bearing). These can be made of either metal on polyethylene plastic (most common) or other bearings such as ceramic-on-ceramic or metal-on-metal.
2. How long will I be in the hospital?
In most cases, patients remain in the hospital at our facility for a minimum of 2 days and usually 3-4 days.
3. Would I go home or go to a nursing facility after the surgery?
This depends on how much help you have at home. The goal of physical therapy both in the hospital and at home is to get you to be independent. If this can not be acheived while you are in the hospital, a vigorous course of therapy in a skilled nursing facility is the best answer to continue to progress toward independence.
4. Can I put my full weight on the leg after a resurfacing total hip replacement?
In most cases of ingrowth prostheses, we restrict the amound of weightbearing on the leg for 4 to 6 weeks. This has been shown to lead to decreased risk of the stem collapsing into the femur
5. What are the advantages of the resurfacing total hip replacement ?
The greatest advantage to the resurfacing hip replacement is the preservation of the patient's bone. By maintaining as much bone as possible in the femoral neck, there is a potential for the bone to continue to be loaded mechanically. This is theorized to lead to increase mineralization in the bone and avoid a complication known as "stress shielding" where the bone that is bypassed with a metal implant is not loaded and can ultimately lose its mineralization as seen by radiographs. Additionally, in the young patient, preservation of the bone can provide increased options in the future in the event of implant failure over the years or in case of trauma.
6. What are its disadvantages?
The biggest disadvantage of resurfacing hip replacement is the exposure of patients to increased levels of metal ions as a result of the metal on metal joint. In spite of higher measured levels of the metal ions, no cases of cancer have been reported directly related to metal on metal hip replacements in spite of greater than 30 years of clinical use.
7. Do resurfacing total hip replacements wear out?
Metal on metal hip replacements such as resurfacing total hip replacements can wear out. Their rate of wear is lower than that measured from standard metal on polyethylene hip replacements. At the current time, it is not known how long the expected implant survival would be for a resurfacing total hip replacement.
8. What kind of activity level can I resume after the resurfacing total hip replacement?
Patients with resurfacing hip replacements are not given any specific activity restrictions. However, just like a standard hip replacment, damage can be done to the hip by excessive activity and impact loading activities. These may ultimately lead to a shorter survival of the implant.
9. Do I have to follow any other precautions after my surgery?
You will be kept on crutches or a walker for the first 4-6 weeks after the surgery unless specified differently by your physician.
10. Do resurfacing hip replacements dislocate?
A dislocated hip can occur during activities in which the precautions are not followed or as a result of soft-tissue laxity or impingement. Impingement is a situation where the component or bony structures contact each other in such a way that they push the hip out of socket. Although resurfacing total hip replacements are very stable and not prone to dislocation, they still can dislocate if the patient goes into a very high degree of bending or twisting at the hip.
11. What about the metal ion issue?
Metal ions are released from every type of hip replacement. Metal on metal bearings such as those used in resurfacing hip replacements are associated with higher levels of metal ions. However, there have never been any cases of cancer directly related to the metal on metal prosthesis in spite of over 30 years of use. We would not recommend metal on metal total hip replacements for patients with liver or kidney disease or the potential for developing such disease.
12. What are the long term results with the resurfacing total hip replacement compared to standard hip replacements?
A number of reports have shown no difference in the early term results between the resurfacing and standard hip replacements. However, resurfacing is technically more demanding and may be associated with more complications. Data from the Australian Hip Registry indicates a higher revision rate in females and in males with smaller stature treated with total hip resurfacing. At this point, it is not clear if the benefits of resurfacing outweigh the risks associated with the procedure.
For more information, see the white paper on Total Hip Resurfacing.
- Schmalzried TP, Fowble VA, Ure KJ, Amstutz HC. Metal on metal surface replacement of the hip. Technique, fixation, and early results. Clin Orthop Relat Res. Aug 1996(329 Suppl):S106-114.
- Tharani R, Dorey FJ, Schmalzried TP. The risk of cancer following total hip or knee arthroplasty. J Bone Joint Surg Am. May 2001;83-A(5):774-780.
- Beaule PE, LeDuff M, Amstutz HC. Hemiresurfacing arthroplasty of the hip for failed free-vascularized fibular graft. J Arthroplasty. Jun 2003;18(4):519-523.
- Jacobs JJ, Hallab NJ, Skipor AK, Urban RM. Metal degradation products: a cause for concern in metal-metal bearings? Clin Orthop Relat Res. Dec 2003(417):139-147.
- MacDonald SJ, McCalden RW, Chess DG, et al. Metal-on-metal versus polyethylene in hip arthroplasty: a randomized clinical trial. Clin Orthop Relat Res. Jan 2003(406):282-296.
- Amstutz HC, Beaule PE, Dorey FJ, Le Duff MJ, Campbell PA, Gruen TA. Metal-on-metal hybrid surface arthroplasty: two to six-year follow-up study. J Bone Joint Surg Am. Jan 2004;86-A(1):28-39.
- Beaule PE. A Soft Tissue-Sparing Approach to Surface Arthroplasty of the Hip. Operative Techniques in Orthopaedics. 2004;14(2):75-84.
- Beaule PE, Dorey FJ, LeDuff M, Gruen T, Amstutz HC. Risk factors affecting outcome of metal-on-metal surface arthroplasty of the hip. Clin Orthop Relat Res. Jan 2004(418):87-93.
- Brodner W, Grohs JG, Bancher-Todesca D, et al. Does the placenta inhibit the passage of chromium and cobalt after metal-on-metal total hip arthroplasty? J Arthroplasty. Dec 2004;19(8 Suppl 3):102-106.
- Graves SE, Davidson D, Ingerson L, et al. The Australian Orthopaedic Association National Joint Replacement Registry. Med J Aust. Mar 1 2004;180(5 Suppl):S31-34.
- Silva M, Lee KH, Heisel C, Dela Rosa MA, Schmalzried TP. The biomechanical results of total hip resurfacing arthroplasty. J Bone Joint Surg Am. Jan 2004;86-A(1):40-46.
- Beaule PE, Antoniades J. Patient selection and surgical technique for surface arthroplasty of the hip. Orthop Clin North Am. Apr 2005;36(2):177-185, viii-ix.
- Clarke IC, Donaldson T, Bowsher JG, Nasser S, Takahashi T. Current concepts of metal-on-metal hip resurfacing. Orthop Clin North Am. Apr 2005;36(2):143-162, viii.
- Davies AP, Willert HG, Campbell PA, Learmonth ID, Case CP. An unusual lymphocytic perivascular infiltration in tissues around contemporary metal-on-metal joint replacements. J Bone Joint Surg Am. Jan 2005;87(1):18-27.
- Grigoris P, Roberts P, Panousis K, Bosch H. The evolution of hip resurfacing arthroplasty. Orthop Clin North Am. Apr 2005;36(2):125-134, vii.
- McMinn DJ, Daniel J, Pynsent PB, Pradhan C. Mini-incision resurfacing arthroplasty of hip through the posterior approach. Clin Orthop Relat Res. Dec 2005;441:91-98.
- Silva M, Heisel C, Schmalzried TP. Metal-on-metal total hip replacement. Clin Orthop Relat Res. Jan 2005(430):53-61.
- Steffen RT, Smith SR, Urban JP, et al. The effect of hip resurfacing on oxygen concentration in the femoral head. J Bone Joint Surg Br. Nov 2005;87(11):1468-1474.
- Treacy RB, McBryde CW, Pynsent PB. Birmingham hip resurfacing arthroplasty. A minimum follow-up of five years. J Bone Joint Surg Br. Feb 2005;87(2):167-170.
- Beaule PE, Campbell PA, Hoke R, Dorey F. Notching of the femoral neck during resurfacing arthroplasty of the hip: a vascular study. J Bone Joint Surg Br. Jan 2006;88(1):35-39.
- Chandler M, Kowalski RS, Watkins ND, Briscoe A, New AM. Cementing techniques in hip resurfacing. Proc Inst Mech Eng H. Feb 2006;220(2):321-331.
- Girard J, Lavigne M, Vendittoli PA, Roy AG. Biomechanical reconstruction of the hip: a randomised study comparing total hip resurfacing and total hip arthroplasty. J Bone Joint Surg Br. Jun 2006;88(6):721-726.
- Graves S, Davidson D, Ingerson L, et al. Australian Orthopaedic Association National Joint Replacement Registry Annual Report. 2006.
- Grigoris P, Roberts P, Panousis K, Jin Z. Hip resurfacing arthroplasty: the evolution of contemporary designs. Proc Inst Mech Eng H. Feb 2006;220(2):95-105.
- Loughead JM, Starks I, Chesney D, Matthews JN, McCaskie AW, Holland JP. Removal of acetabular bone in resurfacing arthroplasty of the hip: a comparison with hybrid total hip arthroplasty. J Bone Joint Surg Br. Jan 2006;88(1):31-34.
- Mont MA, Ragland PS, Etienne G, Seyler TM, Schmalzried TP. Hip resurfacing arthroplasty. J Am Acad Orthop Surg. Aug 2006;14(8):454-463.
- Mont MA, Seyler TM, Marker DR, Marulanda GA, Delanois RE. Use of metal-on-metal total hip resurfacing for the treatment of osteonecrosis of the femoral head. J Bone Joint Surg Am. Nov 2006;88 Suppl 3:90-97.
- Revell MP, McBryde CW, Bhatnagar S, Pynsent PB, Treacy RB. Metal-on-metal hip resurfacing in osteonecrosis of the femoral head. J Bone Joint Surg Am. Nov 2006;88 Suppl 3:98-103.
- Vendittoli PA, Lavigne M, Girard J, Roy AG. A randomised study comparing resection of acetabular bone at resurfacing and total hip replacement. J Bone Joint Surg Br. Aug 2006;88(8):997-1002.
- Amstutz HC, Campbell P, Le Duff MJ. Metal-on-metal hip resurfacing: what have we learned? Instr Course Lect. 2007;56:149-161.
- Beaule PE, Harvey N, Zaragoza E, Le Duff MJ, Dorey FJ. The femoral head/neck offset and hip resurfacing. J Bone Joint Surg Br. Jan 2007;89(1):9-15.
- Beaule PE, Poitras P. Femoral component sizing and positioning in hip resurfacing arthroplasty. Instr Course Lect. 2007;56:163-169.
- Belei P, Skwara A, De La Fuente M, et al. Fluoroscopic navigation system for hip surface replacement. Comput Aided Surg. May 2007;12(3):160-167.
- Cobb JP, Kannan V, Brust K, Thevendran G. Navigation reduces the learning curve in resurfacing total hip arthroplasty. Clin Orthop Relat Res. Oct 2007;463:90-97.
- Davis ET, Gallie P, Macgroarty K, Waddell JP, Schemitsch E. The accuracy of image-free computer navigation in the placement of the femoral component of the Birmingham Hip Resurfacing: a cadaver study. J Bone Joint Surg Br. Apr 2007;89(4):557-560.
- Mont MA, Seyler TM, Ulrich SD, et al. Effect of changing indications and techniques on total hip resurfacing. Clin Orthop Relat Res. Dec 2007;465:63-70.
- Shimmin A, Beaule PE, Campbell P. Metal-on-metal hip resurfacing arthroplasty. J Bone Joint Surg Am. Mar 2008;90(3):637-654.
- Kelley TC, Swank ML. Role of navigation in total hip arthroplasty. J Bone Joint Surg Am. Feb 2009;91 Suppl 1:153-158.
- Kruger S, Zambelli PY, Leyvraz PF, Jolles BM. Computer-assisted placement technique in hip resurfacing arthroplasty: improvement in accuracy? Int Orthop. Feb 2009;33(1):27-33.
- Maguire CM, Seyler TM, Boyd HS, Lai LP, Delanois RE, Jinnah RH. Hip resurfacing-keys to success. Bull NYU Hosp Jt Dis. 2009;67(2):142-145.